In the News
News

Oct 31, 2018
Mental Health and Homelessness
Oct 31, 2018
By Andrew Hening

One of the public’s biggest frustrations related to homelessness is encountering clearly mentally ill individuals living on the street. 44 million Americans – housed and unhoused – experience mental illness every year. Many are medicated or otherwise not outwardly symptomatic, but at times some can sadly display strange, unsettling, or disruptive behavior. This is particularly evident when people are homeless.
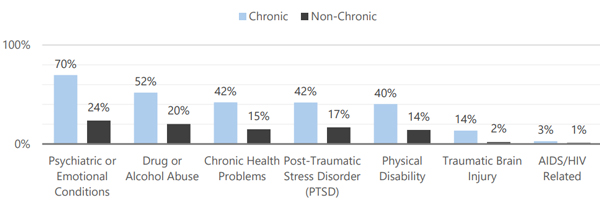
According to Marin’s 2017 Homeless Point-in-Time Count, a staggering 70% of people experiencing chronic homelessness in Marin report having some type of psychiatric or emotional challenge.
WHAT IS SERIOUS MENTAL ILLNESS (SMI)?
The National Institute of Mental Health defines SMI as “a mental, behavioral, or emotional disorder (excluding developmental and substance use disorders) … resulting in serious functional impairment, which substantially interferes with or limits one or more major life activities.”
For this article, we are going to focus on the “big three” diagnoses primarily impacting people experiencing homelessness in San Rafael – major depression, bipolar disorder, and schizophrenia.
Major Depression
Major Depression is characterized by long bouts of profound sadness combined with feelings of hopelessness, chronic fatigue, changes in weight, and poor concentration. Approximately 16 million Americans experience major depression every year.
- Depression is present in at least 50% of all suicides.
- In the US the suicide rate is almost 3x higher than the murder rate.
- Major Depression is thought to result from a decline in serotonin in the brain. Serotonin is a type of neurotransmitter. Neurotransmitters are molecules brain cells use to talk with each other. Other studies suggest depression also stems from social/environmental influences like childhood trauma, loneliness, and a loss of autonomy.
Bipolar Disorder
Formerly known as “manic depression,” Bipolar Disorder is characterized by extended periods of depression AND extended periods of “mania.” Mania is the opposite of depression. It is the belief that one can achieve super human feats, or that one has transformed into a famous or powerful person. Approximately 6 million Americans experience bipolar disorder every year.
- Distorted thinking can lead to outlandish, violent, or generally inappropriate behavior.
- People can completely destroy their lives while in a manic state (e.g. spending all of their savings on erratic purchases or abandoning one’s family.)
- According to Dr. Seager, the author of Street Crazy, the current thinking is that bipolar disorder may be a variety of epilepsy because mania is well controlled by anti-seizure medications.
Schizophrenia
Schizophrenia is a long-term breakdown in the relationship between thought, emotion, and behavior, which can lead to faulty perception, hallucinations, inappropriate actions and feelings, paranoia, delusions of grandeur, and withdrawal from reality and personal relationships into fantasy.
- Approximately 2.5 million Americans experience schizophrenia every year.
- In the US, if you are schizophrenic you have a 5x higher chance of being murdered.
- 10% of schizophrenics commit suicide, and 50% try.
In his book Street Crazy, Dr. Seager says schizophrenia is more than a disease – it is a form of torture. Instead of actually killing you, schizophrenia can cause financial death, employment death, social death, and perhaps most sadly, personality and intellectual death. After onset, a person’s IQ can drop by as much as 45 points.
Research has shown there are really two types of schizophrenia. One type of schizophrenic hears voices, has paranoid disorganized thoughts, but they retain their basic – albeit odd and aloof – personality. Their brain structure isn’t that different (suggesting a possible chemical imbalance), they do well on medications, and with adequate support, can lead a fairly normal life.
The second type of schizophrenic has hardcore, psychotic symptoms. These individuals might be found wearing four layers of ragged clothing on a hot day, they might be found staring blankly and babbling, or they might make outlandish claims of being Jesus or being stalked by the CIA. Brain scans reveal significant structural damage to the brain in these individuals, similar to what happens with dementia.
Anosognosia
Quite amazingly, 70% of schizophrenics respond positively to medication, yet many people, especially among the homeless community, go without. That is because one of the saddest symptoms common to all three diseases is that people cannot even recognize they are ill. The formal medical term for this condition is anosognosia, from the Greek meaning “to not know a disease.”
SUPERNATURAL ORIGINS
For thousands of years mental illness was profoundly misunderstood. Often thought to be witchcraft, demonic possession, or simply moral shortcoming, these misdiagnoses justified a variety of inhumane treatments.
- In 30 AD in Rome, the doctor Celsus argued that philosophy and personal strength were the key to recovery. To that end, he advocated treatments ranging from the wearing of amulets to physical torture.
- In 1483, the Pope sanctioned Malleus Maleficarum (or “Witches Hammer”), which blamed the mentally ill for the Bubonic Plague and justified burning them at the stake.
- According to Dr. Seager’s research, in the 1700s, doctors often thought physical and mental health were connected. As a result, mentally ill patients were submerged in ice water baths, placed in physical restraints, and locked away in isolation.
DOROTHEA DIX
Even though torture, abuse, and ostracization became the standard treatment for centuries, there have been glimmers of hope for more compassionate care.
- The first mental health “asylums” were built in ancient Egypt and Greece. They included boat rides on the Nile and trips to concerts. Asylums were originally seen as havens, shelters, or retreats. They only took on the negative connotation they have today much later.
- For centuries residents of Geel, Belgium, have hosted severely mentally ill people in their homes, simply accepting them as they are.
“Prisons are not constructed in view of being converted into county hospitals, and almshouses are not founded as receptacles for the insane. And yet, in the face of justice and common sense, wardens are by law compelled to receive, and masters of almshouses not to refuse, insane and idiotic subjects in all stages of mental disease and privation.”
10 years before Dix’s remarks’ to the legislature, the US opened its first prison in Philadelphia. The goal of these facilities was penitence, not care-taking. Dix’s solution proposed a new system with a new goal—institutions dedicated to the treatment of mental disorders. By 1880, when the U. S. released its first demographic study of mental illness, forty thousand patients had been moved out of jails and prisons and into state hospitals. Amazingly, only four hundred people with a disorder remained behind bars.
THE FORGOTTEN
In a way, the state hospital system was too successful. People with brain disease had a new place for treatment, and over the next 100 years, successive generations eventually forgot that serious mental illness had ever been such a significant public problem. WWII reopened the issue for two reasons:
- According to Dr. Seager’s research, 40% of all military draft rejections in WWII were for psychiatric reasons. Mental illness did not discriminate against race, religion, or class – it was impacting Americans of all backgrounds.
- There was a huge influx of returning wounded warriors who needed help processing the traumas of war.
Greer Williams, a prominent psychiatrist and writer, was the editor of the final report. In July of 1961, he told The Atlantic:
"Comparatively few of the 277 state hospitals — probably no more than 20% — have actively participated in the modern therapeutic trend toward humane, healing hospitals and clinics of easy access and easy exit, instead of locked, barred, prisonlike depositories of alienated and rejected human beings … [the typical state hospital] does a good job of keeping patients physically alive and mentally sick.”
As public support for state hospitals began to erode, exemplified by books like One Flew Over the Cuckoo’s Nest (1962), with its graphic depictions of electroconvulsive therapy and portrayals of unsympathetic mental-health workers, this period also witnessed astounding progress with the emerging field of psychopharmacology and new drug treatments for mental illnesses. Chlorpromazine, best known in the U.S. under the brand name Thorazine, became the first widely adopted antipsychotic drug in 1955. Others soon followed, and they had an immediate impact on the therapeutic landscape. Although the effects varied from person to person, for the first time many patients with serious mental illnesses could now be reliably treated beyond the asylum and hospital walls.
As a result of all of these developments, when JFK entered the Presidency in 1961, a new vision for mental health treatment was emerging. “We must move from the outmoded use of distant custodial institutions to the concept of community-centered agencies,” JFK told legislators. To replace asylums, the president envisioned a national network of community-based mental health centers, equipped to provide “a coordinated range of timely diagnostic, health, educational, training, rehabilitation, employment, welfare, and legal protection services.” The “Community Mental Health Centers Act” (CMHCA) was the last piece of legislation JFK signed into law before he was assassinated in 1963.
The CMHCA – or “deinstitutionalization” as it is referred to now – was a bipartisan effort with the best of intentions, but the results were not what policymakers envisioned.
THE UNINTENDED CONSEQUENCES OF DEINSTITUTIONALIZATION
If you were to evaluate the success of deinstitutionalization by measuring the clearing out of state hospitals, it was a resounding success. Between 1955 and 1998, the populations in state and county mental health hospitals dropped from approximately 558,000 to fewer than 60,000. If the number of beds available in 1955 had simply kept up with population growth, state hospitals would have had 950,000 patients in 2000. In other words, our country has lost 94% of its per capita mental health bed capacity. Three things happened to accelerate this change.
#1 Medicare and Medicaid
According to research from Dr. Seager’s book Street Crazy, before deinstitutionalization, state hospitals actually served a variety of people, and most people experiencing serious mental illness were being treated and returned home. By comparison, long-term neglect was much more common among senile elderly people and people with incurable, degenerative neurological conditions (epilepsy, ALS, multiple sclerosis, Parkinson’s), who were also warehoused in these facilities.
- In 1965, President Johnson signed Medicare into law. With guaranteed medical insurance regardless of income, elderly patients could finally be moved out of state hospitals to nursing homes.
- In 1966, President Johnson signed Medicaid into law, which provided federal funding for vulnerable people regardless of age. This allowed people with neurological disorders to move to nursing facilities.
- In just 3 years, state hospital populations dropped by 50%.
- Newly funded centers provided easier access for people with anxiety disorders, mild depression, and substance use disorders – problems previously unaddressed by public funding and services.
- Moreover, centers couldn’t handle the behavior of the seriously mentally ill – they didn’t keep appointments and refused medications among other challenges. If there were “easier to serve” people, why attempt to treat those who actively refused treatment or denied they were even ill?
#2 Expanding Civil Liberties
When people are “institutionalized” or “committed,” they are held involuntarily for treatment. There are two legal ideas that support this practice:
- Parens patriae – A legal idea harkening back to medieval English kings whereby the monarch is empowered to be a “substitute parent” for those who can’t care for themselves.
- Police Powers – Grants the government the right to protect society from dangerous individuals.
Building on the momentum of the Civil Rights Movement in protecting individuals’ civil liberties and right to due process, in 1969, California passed the “Lanterman-Petris-Short” Act. In a few short years, the “LPS Commitment Process” became the model law for almost every state.
The LPS Act created strict new standards for involuntary holds that were overseen by the court system. To this day, to be placed on an involuntary hold, someone has to be either:
- An imminent danger to themselves (suicidal);
- An imminent danger to others (homicidal); or
- Gravely disabled (unable to provide food, clothing, or shelter).
- In 1975, in Donaldson vs. O’Connor, the US Supreme Court not only upheld the LPS concept, it went a step further to say no one can be hospitalized involuntarily if that person can simply “survive” in the community.
- In 1979, in Reise v. St. Mary’s in California, the court gave mentally ill people the right to refuse treatment.
- The California Supreme Court has also ruled that past behavior patterns may not be weighed as evidence; instead, involuntary holds must be based on an “imminent” danger.
Pamela grew up in Maryland. After a relatively uneventful childhood, as a young woman Pamela had a violent, psychotic break during which she stabbed her mother 47 times. At her trial Pamela indicated voices had compelled the attack, and she was sent to a state hospital. Amazingly, she was released after just one year. With her new freedom she got on a bus and headed to Los Angeles. After arriving in LA, Pamela’s schizophrenia began to encourage self-mutilation, and over the next couple years Pamela cut off the tips of all of her fingers, toes, nose, and ears. This self-endangerment landed her in psych emergency 49 times. Every time Pamela started taking medication, her condition improved, and she was released. Once Pamela felt partially well again, she stopped taking her medication. On that 49th visit, Pamela had gouged out one of her eyes.
#3 Defunding Mental Health Services
Even though the 1960s witnessed massive investment in publicly-funded healthcare through Medicaid and Medicare, the Community Mental Health Act of 1963 was immediately gutted of its major funding provisions. The American Medical Association opposed including funds for personnel, and in the final bill nothing was set aside for staffing.
In the last year of his presidency, Jimmy Carter signed the Mental Health Systems Act (MHSA) of 1980, which provided more grant funding directly to community mental health centers. However, even after John Hinkley, Jr. – a man suffering from an untreated psychotic disorder – attempted to assassinate President Reagan in March of 1981, Reagan went on to repeal most of MHSA later that same year.
By the mid-1980s, it was apparent that something had gone wrong:
The Great Recession accelerated the nation’s downward trend in mental-health spending. Between 2009 and 2012, America’s 50 state legislatures cut a total of nearly $4.5 billion in services for the mentally ill, even as patient intakes increased by nearly 10% during the height of the economic crisis.
TODAY
It is now believed that 1/3 to 1/2 of all inmates in the US have a mental illness. That’s 400,000 people. The largest mental health facility in the country is now the Cook County Jail in Chicago. The National Alliance on Mental Illness estimates that between 25 and 40 percent of all mentally ill Americans will be jailed or incarcerated at some point in their lives.
Most mentally ill inmates end up behind bars because of “crimes of survival” such as retail theft (to find food or supplies) or breaking and entering (to find a place to sleep). For those with mental illness, drug possession charges can often indicate attempts at self-medication. The 1976 Supreme Court case Estelle v. Gabriel found that prisons are constitutionally required to provide adequate medical care to inmates in custody, thus creating a potentially perverse incentive to commit crimes to receive treatment.
Like it was in the 1800s, jail continues to be a terrible place for people with mental health issues. In Insane, Elissa Roth visited prisons across the country, observing mentally ill people without access to medication, constantly surrounded by loud noises and sounds, in tight confined spaces, sleep deprived, and often in isolation. Mentally ill inmates fail to understand the rules they’re expected to follow or the punishment they receive, and their conditions result in the exact opposite behavior of what correction officers desire – paranoia and noncompliance.
This depressing state of affairs was not inevitable. It is the direct result of decades of policy decisions to stifle the community health mental vision. But that original vision is still sound. And there is reason to hope that one day we will fully implement it.
This article was originally published by The City of San Rafael in a three part blog. Reprinted here with permission.
Andrew is the Director of Homeless Planning & Outreach for the City of San Rafael. Andrew provides strategic focus to the City’s efforts to address homelessness. He has strengthened relationships with community members and he has worked in collaboration with local partners to spearhead innovative new pilot programs and initiatives. To learn more visit the City’s blog. Andrew.hening@cityofsanrafael.org












